
Every year, without fail, I start having the same conversation.
It’s usually said almost apologetically.
“I know it’s only hayfever…”
But it isn’t “only” anything when you haven’t slept properly in weeks. When your sinuses feel permanently inflamed. When your head feels heavy and your energy dips every afternoon. When you’re juggling work, family, responsibilities - and on top of that, your body is reacting to pollen as if it’s under attack.
Hayfever is common. That doesn’t make it insignificant.
For most people, antihistamines and nasal sprays are enough. For some, they aren’t. And that’s usually the point where patients start searching online for something stronger.
That’s often when they come across the phrase “hayfever injection”.
And this is where things need to be handled carefully.
Seasonal allergic rhinitis isn’t just sneezing.
It’s an inflammatory cascade.
When pollen comes into contact with the lining of the nose or eyes, the immune system releases inflammatory mediators. Histamine is one part of that response - but it isn’t the only one. In more significant cases, the inflammation becomes broader, deeper and more persistent.
The nasal lining swells. Mucus production increases. Sinuses feel pressured. The body stays in a low-grade inflammatory state.
And when that inflammation doesn’t settle with standard treatment, it can become draining.
This is the point where escalation is sometimes discussed.
One of the biggest misconceptions about private hayfever care is that it’s a shortcut.
It isn’t.
Prescription anti-inflammatory injections - specifically systemic corticosteroids - are powerful medicines. They work by suppressing immune activity throughout the body, not just in the nasal passages.
That broader effect is exactly why they must be approached cautiously.
These injections are not first-line treatment. They are not suitable for everyone. And they are not routinely commissioned within NHS primary care for hayfever.
Private consultation simply allows time for a detailed assessment to determine whether the severity of symptoms justifies the potential risks.
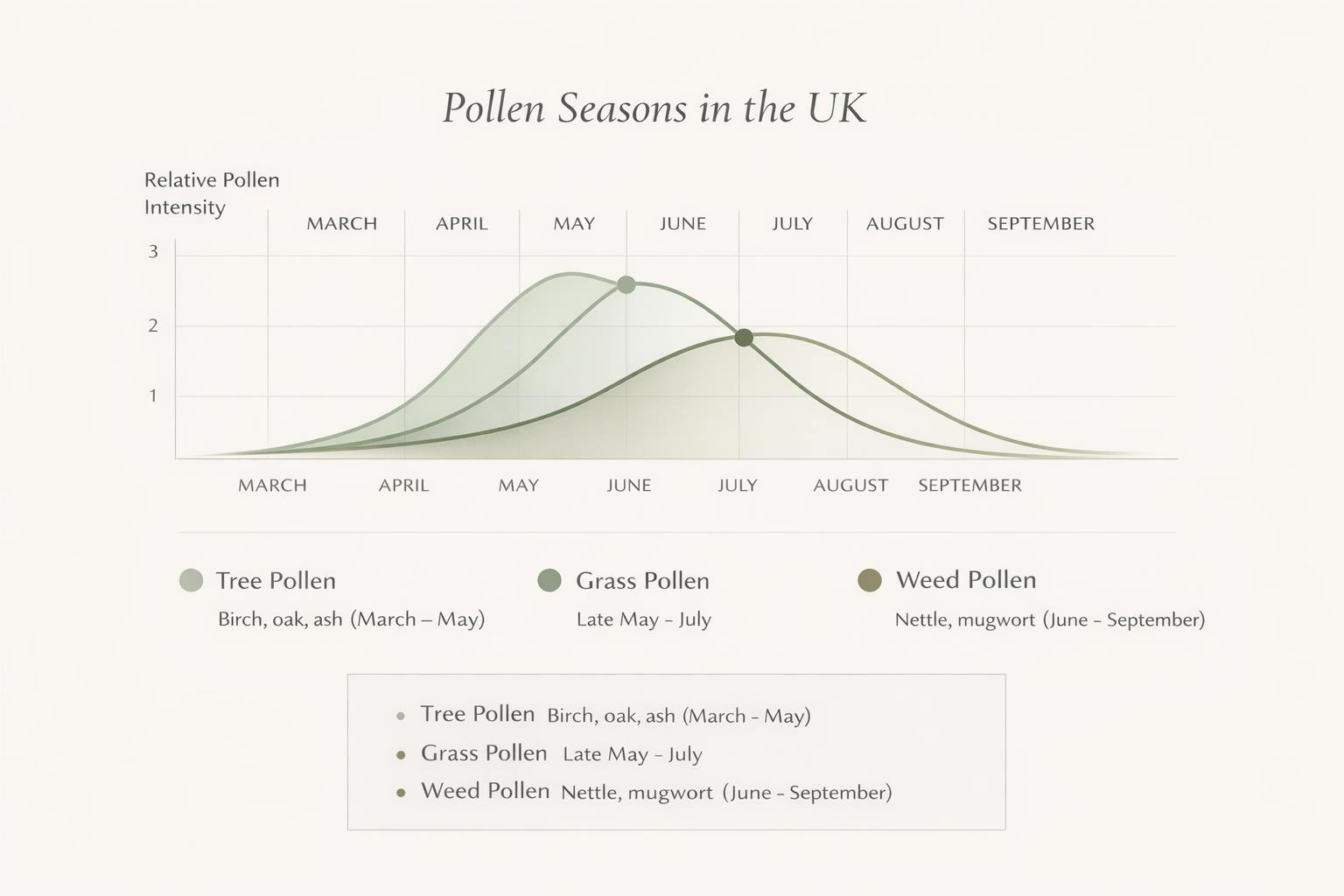
One of the reasons hayfever feels unpredictable is because “pollen season” isn’t one single event.
In the UK, we actually move through three distinct pollen waves - and symptoms can shift depending on which type you’re reacting to.
Tree pollen is usually the first to appear, often beginning in March and peaking through April and early May.
Common triggers include birch, oak and ash.
This is the period when many people experience sudden onset symptoms after a relatively symptom-free winter. It often presents as:
Because tree pollen arrives early, patients are often caught off guard. They haven’t started medication yet, and inflammation builds quickly.
In Manchester, tree pollen levels can rise earlier in milder springs, particularly after dry, windy weather.
Grass pollen is the most common cause of hayfever in the UK.
It typically peaks between late May and July and is often responsible for more persistent and heavier symptoms.
During grass pollen season, inflammation can feel deeper and more sustained. Patients frequently report:
Because grass pollen levels can remain high for several weeks, symptoms often feel relentless during this phase.
If hayfever tends to affect you more severely, it is often during grass pollen season.
Weed pollen appears later, usually from June through September.
Common sources include nettle and mugwort.
This stage can prolong symptoms just as people expect relief. For some, it feels like hayfever simply never switched off after grass season ended.
Late-season symptoms are often milder but persistent, with ongoing congestion and irritation rather than dramatic flare-ups.
Different pollen types trigger slightly different inflammatory responses. You might notice that early spring feels more eye-dominant, while early summer brings heavier nasal congestion.
Weather also plays a role.
Warm, dry, windy days increase airborne pollen levels. Rain can temporarily reduce airborne pollen, but humid conditions can worsen congestion.
This is why symptoms don’t always follow a neat calendar.

Before I would ever consider prescribing a systemic corticosteroid for hayfever, we go through a full clinical review.
That includes:
The consultation process is important so that you can understand the risks involved.
Because systemic corticosteroids suppress immune activity beyond the nose and sinuses. They can affect blood sugar. Blood pressure. Mood. Sleep. Hormonal patterns. Skin integrity. In rare cases, more serious complications can occur.
Those risks need to be weighed against the severity of symptoms.
Sometimes that balance supports treatment.
Sometimes it doesn’t.
And sometimes, after understanding the full picture, a patient chooses not to proceed. That’s entirely appropriate.
Responsible prescribing isn’t about saying yes.
It’s about making proportionate decisions.
If someone’s symptoms are genuinely severe, affecting sleep, concentration and daily function, and they have no medical contraindications, systemic treatment may be considered.
If their symptoms are moderate, or risk factors are present, the safer option may be optimisation of existing treatment or exploring alternatives.
Private care should never mean relaxed standards.
If anything, it requires greater caution.
There’s a lot of noise online about hayfever injections.
What’s often missing from that conversation is nuance.
Prescription corticosteroids are established anti-inflammatory medicines used across multiple areas of medicine. They are effective in certain contexts. But they are not benign. And they are not appropriate for everyone.
That’s why at House of Glo, hayfever care always begins with discussion, examination and risk assessment.
You may consider booking a consultation if your symptoms are persistent, worsening year on year, or no longer responding to standard over-the-counter treatments. If sleep, concentration or daily functioning are affected during pollen season, a medical review can help clarify your options.
Hayfever may be considered moderate to severe if you experience constant nasal obstruction, prolonged sinus pressure, disrupted sleep, or reliance on multiple medications daily with limited improvement. Severity is assessed individually during consultation.
If antihistamines and nasal sprays no longer provide adequate control, it’s reasonable to seek medical advice. Sometimes treatment optimisation is sufficient. In other cases, further assessment may be needed to evaluate whether alternative management strategies are appropriate.
Not necessarily. A prescription injection is not automatically indicated when symptoms persist. A full medical consultation is required to assess overall health, risk factors and whether any escalation of treatment is clinically justified.
Yes, symptom patterns can change over time. Some people find their reactions intensify during certain pollen seasons, particularly grass pollen. A review can help determine whether changes in management are needed.
That depends on your medical history and previous treatment response. For prescription treatments, regular reassessment is important to ensure continued suitability and safety.
A structured consultation includes review of symptom history, current and past treatments, nasal spray technique, asthma screening, blood pressure measurement, medication review and discussion of any medical risks. This ensures any treatment decision is proportionate and safe.
Private care does not change prescribing standards. All treatment decisions are based on medical suitability, risk assessment and informed consent.
The goal isn’t to push treatment.
The goal is clarity.
And sometimes clarity alone reduces the urgency people feel when they’ve been struggling for weeks.
If you’d like a medically led hayfever consultation in Manchester, you can arrange one here. We offer in person, or online consultations - whichever you prefer!
> Book a consultation
Stay in the glow - sign up to the House of Glo newsletter to receive exclusive offers, updates, and beauty tips straight to your inbox!